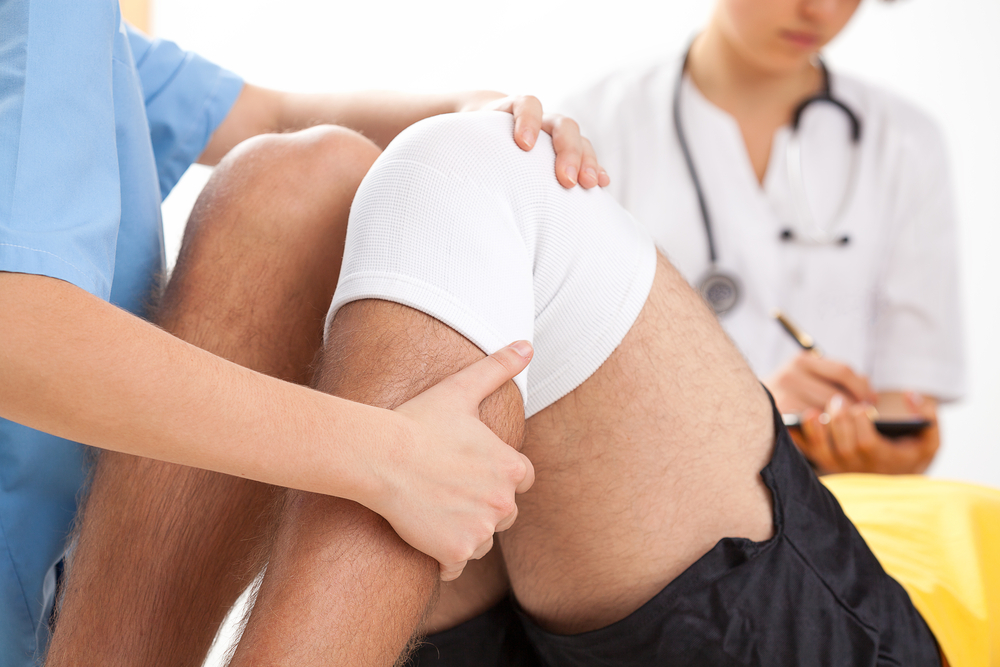
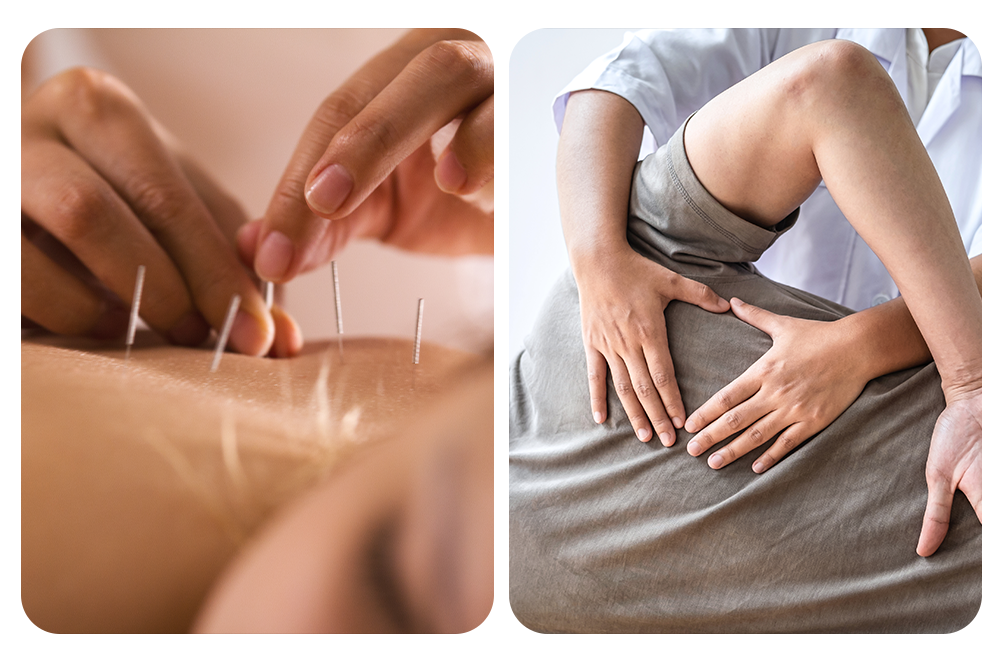
Why Some Injuries Never Seem to Heal (and What Physio Can Do Differently)
There’s nothing more frustrating than an injury that just won’t go away. It gets better, then flares up again. You rest it, then it hurts the moment you’re active. You’ve […]
Why Some Injuries Never Seem to Heal (and What Physio Can Do Differently) READ MORE »